No content results match your keyword.
Content
You have successfully logged out.
Not registered yet?
Smart hospital
How will a hospital operate in the year 2040? A tour through the health care system of the future.
As Karla suddenly slumped down at lunch, her colleagues were naturally alarmed. But they didn't call an ambulance, they just carefully sat Karla up. This is because she was wearing a first responder right on her body: her undershirt. The smart clothing uses interwoven sensors to measure EKG information, heart rate and skin conductance, then uses software to factor in Karla's health information, such as preexisting conditions and genetic characteristics. The software detects a threatening situation - a heart attack - and sends this assessment to Karla's smartwatch, which then flashes red like a stop light. An ambulance is on the way.
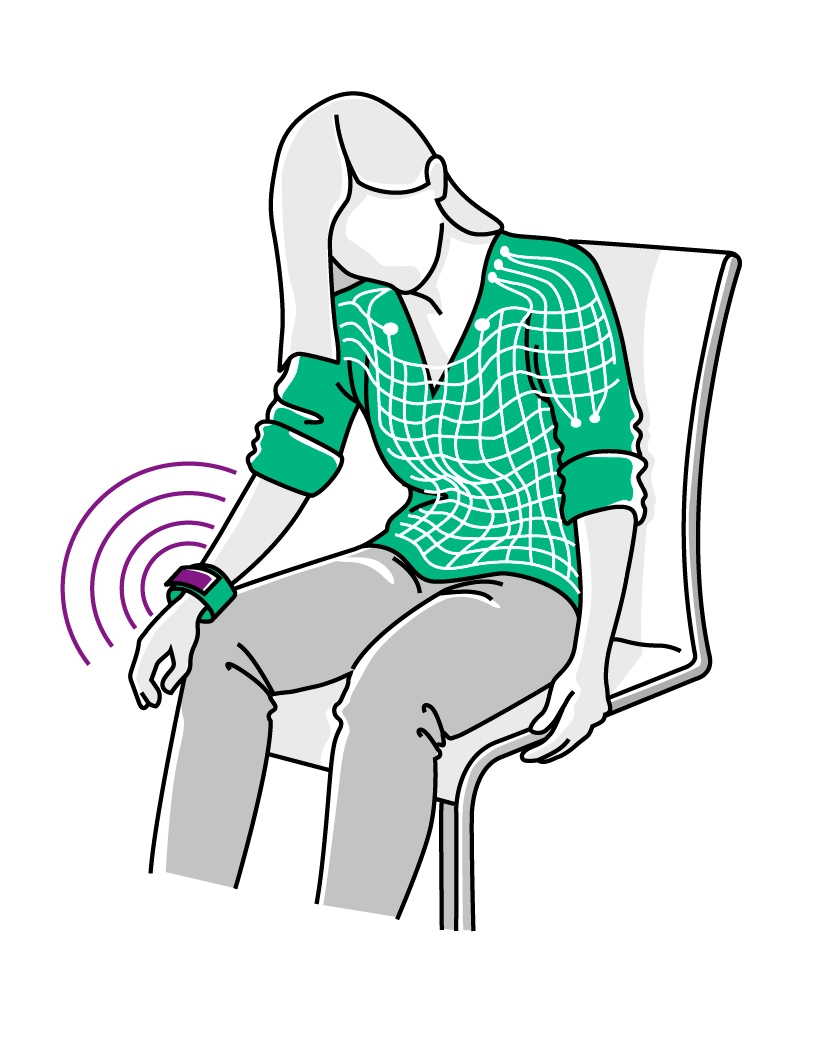
Karla is a fictional person. She lives in the year 2040 in a central European city and is 45 years old. She is a non-smoker, is active in sport and is a flexitarian – a quite normal diet in the year 2040 in urban settings. Yet in the future people still suffer from stress. Karla also has a genetic pre-disposition that increases her risk of cardiovascular disease. And now it has happened: Heart attack. Emergency lights. Hospital. But what is it like for a sick person in the year 2040? Does the health care system operate exactly the same way as today? We are going to take a tour with Karla of the hospital of the future.
"I am an optimist. I believe that a major problem with the health care system will have disappeared in ten to twenty years", says Burkhard Rost, a professor of bioinformatics at the Technical University of Munich, who is a researcher in the field of computational biology. Currently strict data privacy laws still prevent the networking of all the actors in the health care system. "Hospitals, doctors and even individual departments inside the hospital can barely communicate and exchange data with each other", says Rost. But he believes that it will soon be possible to tap into the vast wealth of data that currently exists – blood test results, hereditary dispositions, data from experiments, studies or smartphone apps. "In the field of molecular medicine, more data was generated in the year 2015 than over the entire period from 1990 to 2005", says Rost.
Each year the volume of all medical data grows exponentially in which researchers and doctors could discover interconnections and cures if they were able and authorized to use the data. Patients today therefore often have to undergo tests many times. "For this reason, we lose valuable resources and time while a patient is suffering", says Rost.
“If in the year 2040 the data can circulate, with appropriate protections against misuse, and is available for doctors and care givers at any time, this will change almost everything in the medical field.”
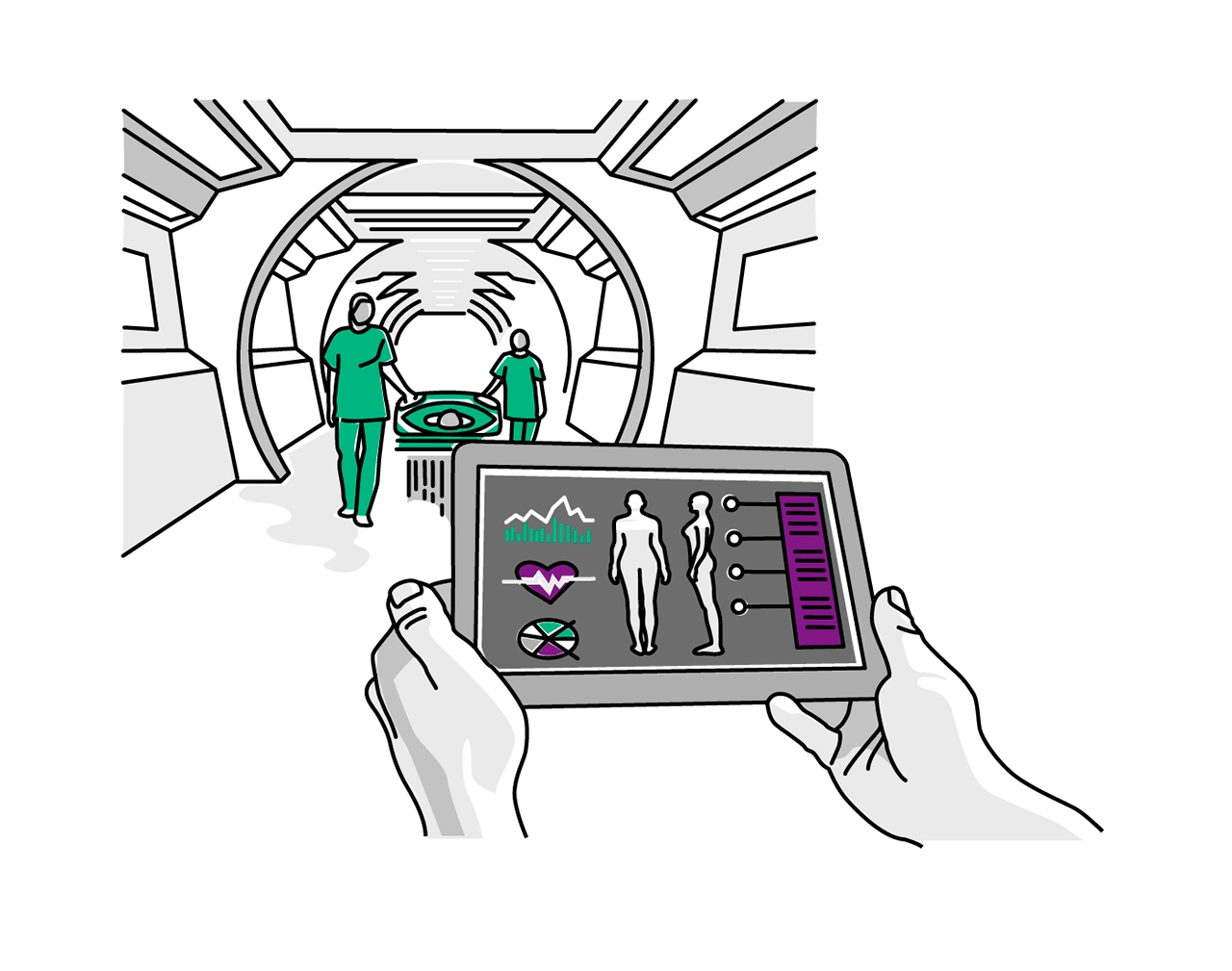
Karla has now arrived at the hospital. No one has to stop to fill out lists or create a patient record there. The doctors have already studied all important information about Karla on their tablet or smartphone before she even arrives – including a comprehensive EKG analysis that Karla's undershirt has been tracking for months. In the year 2040, each medical institution no longer individually saves its data on a patient. A digital patient file is available for doctors at all times and anywhere. Doctors will also use special software and global databases to obtain information, such as a cancer registry. There they can compare their diagnosis with other cases worldwide. The patient can also benefit: The undershirt had already warned Karla of a possible heart attack two days before because the sensors registered changes in her EKG. The fact that she didn't go to the doctor was her own personal negligence.
"Today radiologists overlook 11-14 percent of prostate cancer cases on the first radiological test", says Maximilian Waschka, founder of the start-up Fuse-AI. "With software that uses artificial intelligence, the error rate can be reduced to one percent." The 25-year old Waschka is developing with his colleagues a software that goes through MRT images of prostate carcinomas and pre-marks cell accumulations that it judges to be cancer. Next year the software will go on the market – and make diagnoses more reliable. "Today a radiologist has to look through a thousand individual images for each MRT scan before making a diagnosis. This takes approximately 30 minutes".
Using his software, it would just be a quarter of an hour. For Karla, this means above all: Her diagnosis is on significantly more solid ground than today. She also gets the right treatment faster, which greatly affects the chances of recovery, especially with diseases like cancer or a heart attack. Because Karla is in the hospital in such a short time, her chances are very good that the tissue of her heart muscle that dies will be minimal – and she will not suffer from chronic cardiac insufficiency later.
Hospitals are often like huge labyrinths, where most people feel lost. Endless halls, cold neon light, five different elevators – and nobody knows where the surgery department is. But it is also important for nurses, doctors and planners that people and material get from point A to B as quickly as possible. Time is an enormously important factor in the health care system. "We now build hospitals so that the flow of people and goods can move as quickly and efficiently as possible", says Carolina Lohfert Praetorius. Lohfert, who is a doctor and hospital planner, has already built hospitals in Scandinavia, Germany, Austria and Switzerland with her company Lohfert – Praetorius A/S and she is familiar with both old and new standards.

"Old hospitals frequently have a pavilion structure: The departments are widely scattered over individual, small buildings on the hospital grounds", says the doctor from Copenhagen. "But this is inefficient. Often you have to go from one department to the other by car." In addition, there are frequently also trouble spots where product and human flows have concentrated. "You'll see a garbage truck next to the visitors and the acute patients." If things go as she envisions, such possible sources of error and wasted time will no longer exist in the hospital of the future. Within minutes of arrival in the emergency room, Karla is on her way to the operating room and does not have to change buildings. "Departments and hospitals are being designed more compactly, so that everything that should be connected can be found in one building", says Lohfert Praetorius. "For reasons of cost and efficiency, the trend is towards centralization." In the year 2040 there will probably be fewer hospitals.
“But the ideal is for these centers to be able to run more efficiently and to specialize in particular specialist areas. In this way the quality of treatment is improved.”
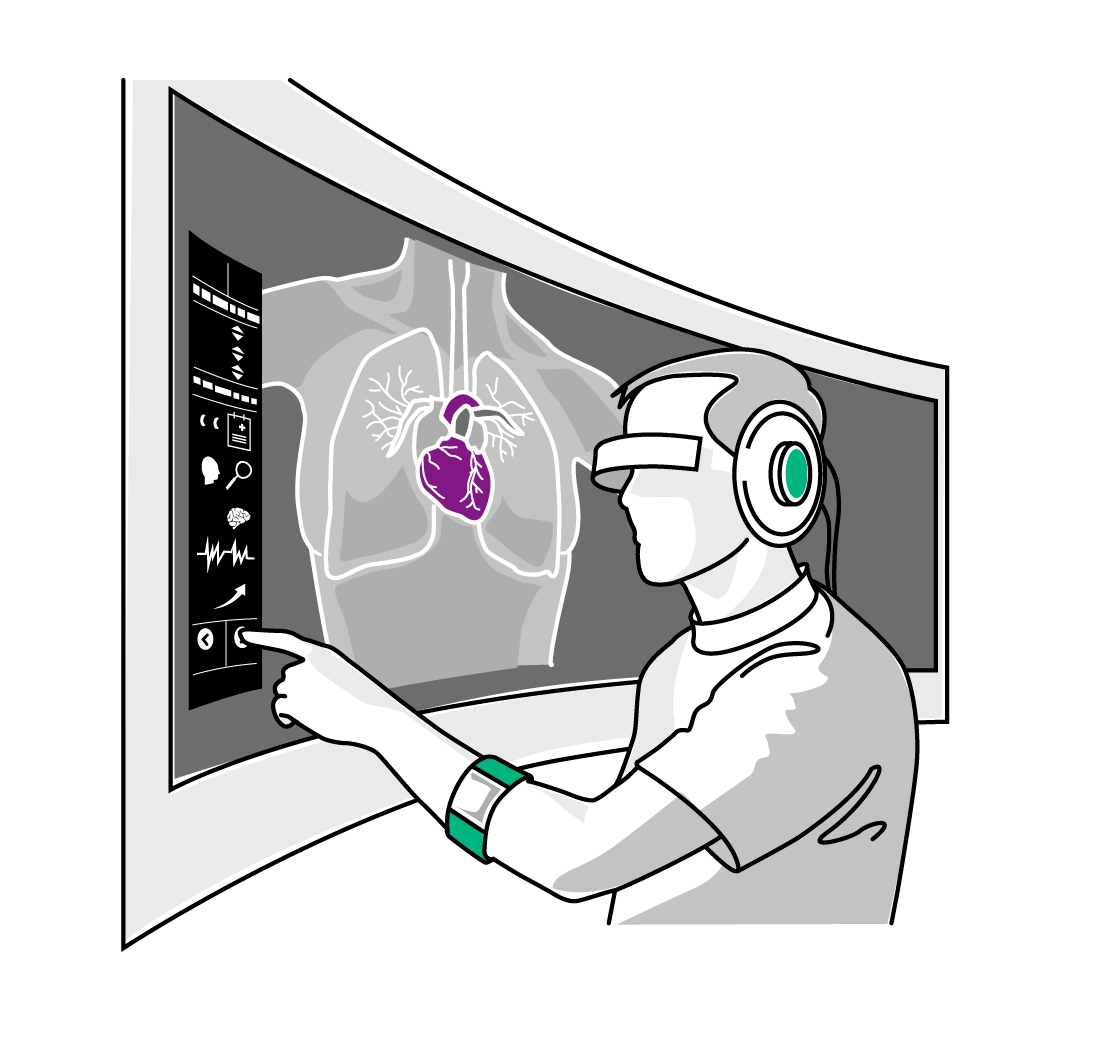
Karla has gotten to the operating room at great speed. To an observer from today, the room would look strikingly empty. The operating room of the future will get by with significantly fewer devices. There will be no large monitors for MRT images or x-ray tubes, for example. The surgeon could well be practically alone. On the integrated screen of a pair of smart glasses, the surgeons will be able to zoom in on the patient and individual body parts and will have all the important information in front of them on a single screen. Because software had already decoded Karla's genome years ago, the doctors were able to select the operating method that was clearly best for her genetic type. Before beginning, Karla's surgeon checks the programming of the surgical robot.
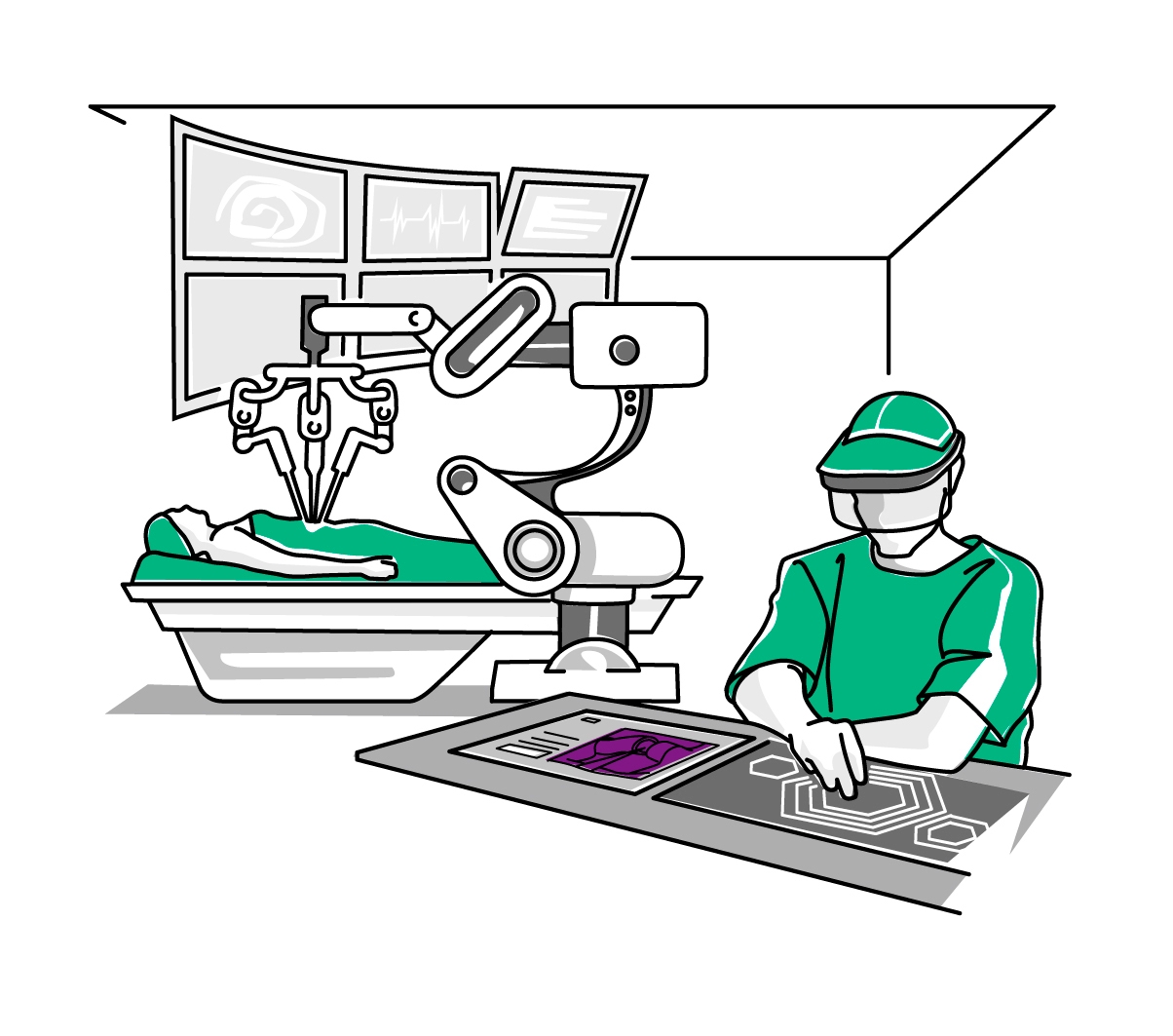
“In the future doctors will certainly routinely work with fully automated surgical robots in many clinical indication fields.”
"We will see a routinized type of teamwork between humans and machines." Even today the robot-assisted operating system Da Vinci is increasingly replacing the traditional method of surgical prostatectomy. Humans control Da Vinci with a joystick, which translates this input into extremely delicate incisions. The goal is for the patients to experience less frequent pain and incontinence after such operations and to lose less blood. Operating times should also be significantly reduced in the future. "In addition, in the year 2030 implants such as artificial joints will be combined with sensors which will, for example, inform the patient of peak exertion during different sports activities or if necessary, dispense medications in the event of local inflammatory responses", says Sternberg. "3D printers modulate perfectly fitting implants for individual patients." For Karla, this means: Her stent itself, which an operating system inserts with maximum precision and minimal blood loss, gives off active agents – and sends a message to the doctor's smartphone if complications arise.
Karla is not aware of any of this. She is still under anesthetic. But otherwise she wouldn't notice a tremendous change between a hospital visit today and one in the year 2040. "For a patient, the changes will not be very noticeable, as with an airline passenger that isn't aware of all the processes that run during an Atlantic flight", says Jochen Werner, CEO and Medical Director at the Essen University Hospital. He developed a master plan for his hospital and is currently transforming it into a smart hospital. "At most the patient might notice that there are far fewer disruptions, wait times and problems", says Werner.
When Karla wakes up in the hospital bed, she is alone in a spacious room, with a large window facing the south. In the year 2040, there will be far more single rooms and more comfortable accommodations than today. "When people have plenty of light, are undisturbed and sleep well, they just recover faster", says hospital planner Lohfert Praetorius. "And shorter stays in the hospital benefit both the patient – because they can go home sooner – and the health care system."
The hospital of the future has a completely new operating system. This is because the modern treatment methods, the generous and better accommodations and the modern, individual gene medications naturally have their price. "But I'm sure that with digitization, the introduction of the electronic patient file, shorter operating and hospital times and less frequent misdiagnoses from genetic analyses, there will be sufficient cost savings to make these improvements possible", says hospital director Jochen Werner. Studies show that with the resources already available today, up to 35 billion euros could be saved – just from the consistent use of the digital resources that already exist. At the Essen University Hospital, for example, many projects are being combined using artificial intelligence based on modern IT systems to create a "Medical Cloud", which as a core element of the smart hospital also includes the entire pre- and post-treatment area.
“I am convinced that digitization will help doctors fulfill their key task: helping and curing people.”
Karla is experiencing pain, feels anxious, unwell. She calls for a nurse practitioner. He appears immediately – on a screen. A camera films Karla, and the nurse can also see her. "What can I do for you?" he asks. "I'm feeling pain. Where am I?", asks Karla. The nurse reassures the patient. He observes Karla's condition on his tablet, monitors the administration of medicine, and Karla is given more pain medications. "Dr. Kluge will be there soon to see you, it will just be a few minutes", the nurse assures her.
“In the future, the use of apps and telemedicine will be entirely common.”
The professor of health psychology at the Leuphana University Lüneburg is an expert in the field of eHealth and develops apps and online programs for patients with psychological illnesses. Patients in the year 2040 will have far fewer and shorter hospital stays than in 2019. Online programs, apps and smart watches will help them prevent illness and recover from them – and focus on making progress, according to Lehr. In Karla's specific case, that could mean that she learns to reduce stress. In a virtual reality that reconstructs her work environment, she might practice situations where she negotiates with her boss for more free time and more effectively sets boundaries.
There is a chance that for the patient of the future, things will be better in the hospital than today. Because he is treated better, because the chances of a cure will be greater, because doctors and nurse practitioners will be more responsible to his personal needs. "This will also be noticeable in the details – such as the privacy and the food", says hospital planner Lohfert Praetorius.
Karla is hungry. She logs in to the hospital network on her tablet and looks through the different menu options for a chicken soup, a dish she's hungry for. Anyone who has ever eaten in a hospital before knows what a step forward that is.
Your feedback matters! Participate in our customer survey to help us enhance our website, products and services. Thank you for your support!