No content results match your keyword.
Content
You have successfully logged out.
Not registered yet?
Experience Report
Dr. med. Mirko Otto, Acting Senior Physician, Surgical Clinic, Mannheim University Medical Center
The bariatric operations performed fall mainly into two types: laparoscopic sleeve gastrectomy (LSG) and laparoscopic Roux-en-Y gastric bypass (RYGB). The currently available data shows that the two procedures are equivalent to one another, at least in the initial post-operative years. [5] There is currently no long-term data for the subsequent years. There is a loss of around 60-70% of the overweight and a clear improvement in concomitant diseases.
These two procedures also account for the majority of the bariatric operations performed at our clinic as well, as we can achieve good results with lower morbidity with these procedures. Based on the available longterm data (over 10 years), we first recommend the RYGB if there are no contraindications. Contraindications include chronic inflammatory bowel diseases, conditions following kidney transplantation with significant medication dependency and prior major intestinal surgery.
The number of additional procedures with evidence of good effectiveness is increasing. So, the single-anastomosis gastric bypass (omega loop), the biliopancreatic diversion with a duodenal switch (BPDDS) and even the gastric band should not be left unmentioned.
The omega loop is a real alternative for patients with a BMI of 50-60 kg/m2 as it leads to better weight loss compared to the two traditional procedures. Unfortunately, the development of a gastric stump carcinoma cannot be ruled out, which is why young patients should be advised against undergoing this procedure. [6]
For very heavy patients (BMI > 65 kg/m2), often only one multistage process is considered. After initial sleeve gastrectomy, BPDDS seems to the have the best weight loss results with a concomitant excellent effect on any possible diabetes. Quality of life, measured using a questionnaire (BAROS) on physical, social and psychic effects is significantly improved after the operation, despite the malnutrition caused by the operation. [7]
The gastric band provided excellent data in an Australian study. However, the requirement for intensive follow-up care, which is not paid for in Germany, is problematic. Therefore, this procedure is rare both in Germany and at our clinic. [8]
Different methods can also be combined in individual cases, e.g. the fitting of a gastric band to an existing gastric bypass (laparoscopic banded Roux-en-Y-gastric bypass). However, this should be a strictly exceptional indication as there is no long-term data available, there are no prospective randomized superiority studies and the negative effects of a foreign body are already known about from the traditional gastric band.
Every indication and each surgical procedure requires an individual decision, agreed with the patient. From our perspective, the good long-term data and good tolerability of LSG and RYGB support the use of these procedures. A general recommendation for the other methods cannot be given due to the lack of evidence regarding their equivalence.
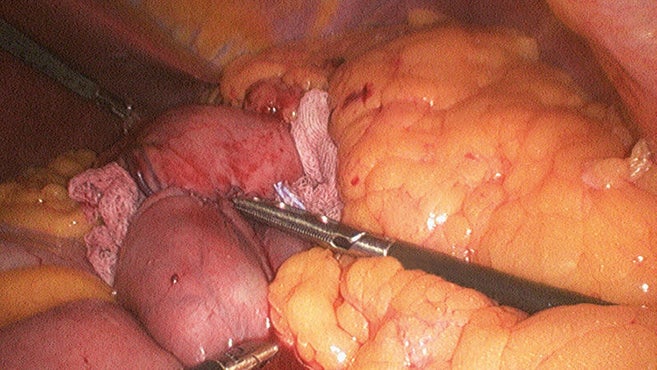
Indigo carmine test following gastrojejunostomy
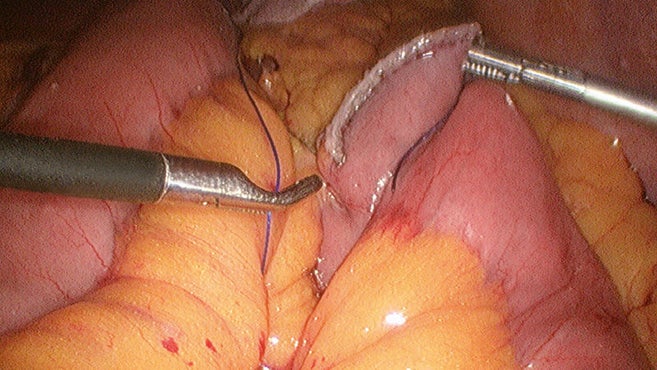
Closure of the mesocolon opening after stapling of the jejunojejunostomy

Acting Senior Physician, Surgical Clinic
[1] Sjöström L, Lindroos AK, Peltonen M, Torgerson J, Bouchard C, Carlsson B, Dahlgren S, Larsson B, Narbro K, Sjöström CD, Sullivan M, Wedel H. Swedish Obese Subjects Study Scientific Group. Lifestyle, diabetes, and cardiovascular risk factors 10 years after bariatric surgery. N Engl J Med. 2004 Dec 23;351(26):2683-93.
[2] Buchwald H, Oien DM. Metabolic/Bariatric Surgery Worldwide 2011. Obes Surg. 2013 Jan 22 (Epub ahead of print).
[3] Lassailly G, Caiazzo R, Buob D, Pigeyre M, Verkindt H, Labreuche J, Raverdy V, Leteurtre E, Dharancy S, Louvet A, Romon M, Duhamel A, Pattou F, Mathurin P. Bariatric Surgery Reduces Features of Nonalcoholic Steatohepatitis in Morbidly Obese Patients. Gastroenterology. 2015 Aug;149(2):379-88; quiz e15-6. doi:10.1053/j.gastro.2015.04.014. Epub 2015 Apr 25.
[4] German Federal Statistical Office.
[5] Peterli R, Borbély Y, Kern B, Gass M, Peters T, Thurnheer M, Schultes B, Laederach K, Bueter M, Schiesser M. Early results of the Swiss Multicentre Bypass or Sleeve Study (SM-BOSS): a prospective randomized trial comparing laparoscopic sleeve gastrectomy and Roux-en-Y gastric bypass. Ann Surg. 2013 Nov;258(5):690-4; discussion 695.
[6] Victorzon M. Single-anastomosis gastric bypass: better, faster, and safer? Scand J Surg. 2015 Mar;104(1):48-53.
[7] Ballesteros-Pomar, González de Francisco, Urioste-Fondo, González-Herraez, Calleja-Fernández, Vidal-Casariego, Simó-Fernández, Cano-Rodríguez. Biliopancreatic Diversion for Severe Obesity: Long-Term Effectiveness and Nutritional Complications. Obes Surg. 2015 May 17. [Epub ahead of print]
[8] Burton, Brown, Chen, Shaw, Packiyanathan, Bringmann, Smith, Nottle; Outcomes of high-volume bariatric surgery in the public system. ANZ J Surg. 2015 Oct 16.
[9] Chaux F, Bolaños E, Varela JE. Lengthening of the biliopancreatic limb is a key step during revisional Roux-en-Y gastric bypass for weight regain and diabetes recurrence. Surg Obes Relat Dis. 2015 Nov-Dec;11.
[10] Aghajani E, Jacobsen HJ, Nergaard BJ, Hedenbro JL, Leifson BG, Gislason H; Internal hernia after gastric bypass: a new and simplified technique for laparoscopic primary closure of the mesenteric defects. J Gastrointest Surg. 2012 Mar;16(3):641-5.
Your feedback matters! Participate in our customer survey to help us enhance our website, products and services. Thank you for your support!