No content results match your keyword.
Content
You have successfully logged out.
Not registered yet?
The challenge in chronic wounds
In developed countries, it has been estimated that 1 to 2% of the population will experience a chronic wound during their lifetime.1 Wound infections are one of the most frequent complications of non-healing wounds2 and represent a challenge for patients, healthcare professionals and institutions.

They can compromise the healing process with a significant negative impact on health-related quality of life.3 Patients with an infected wound typically experience discomfort with symptoms such as pain, unpleasant odor, purulent exudate, reduced mobility, among others.4 Challenges that deeply can affect both patients and their families.5
Management of infected wounds requires a multidisciplinary team and a holistic approach that includes comprehensive wound assessment and overall patient care.6 It is therefore essential to identify the most effective strategies to prevent, diagnose, and manage them properly.
0 to 2%
of the population will experience a chronic wound during their lifetime.7
More than
0%
of chronic wounds are estimated to be infected.8
The wound infection continuum looks at the different stages of wound infection progressing from initial contamination up to overt sepsis.9,10 This concept, provided by the International Wound Infection Institute (IWII) is designed to support healthcare professionals in identifying the right strategies for preventing and managing infected wounds.
*The use of Prontosan and Askina does not replace the need for systemic or other specific infection treatment. Adapted from International Wound Infection Institute (IWII) Therapeutic wound and skin cleansing: Clinical evidence and recommendations. Wounds International. 2025.
Click here to download the full graphic for your reference.
Download nowAn advanced combined approach
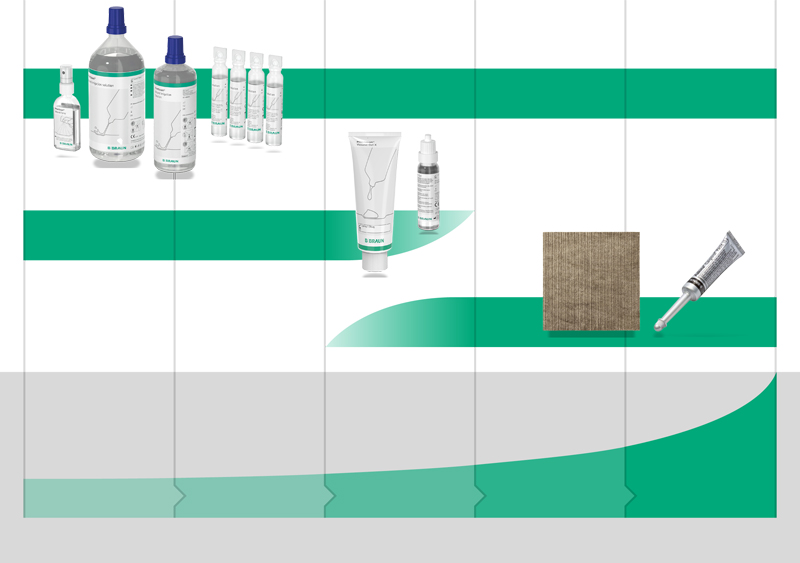
Our therapy concept covers all stages of the wound infection continuum with our recommended solutions. Prontosan® Irrigation Solution for therapeutic wound cleansing to prevent biofilm formation from the initial to the final stages of the continuum. Prontosan® Wound Gel and Wound Gel X support the prevention of infection by providing an antimicrobial barrier.
For the treatment phase, our Askina® Calgitrol® range of silver wound dressings designed to treat infected wounds, reduce the clinical signs of infection11 while providing a broad antimicrobial effectiveness.12 Evidence shows that using a biofilm remover/cleanser together with an antimicrobial agent is more effective in managing infection than using an antimicrobial alone.13
Our commitment is to support clinicians with effective, well‑tolerated options that lower infection risk, antimicrobial resistance and create the ideal environment for wound healing — leading to better outcomes and more efficient care.
Prontosan® markedly reduces infection rates over time14-16 and outperforms saline17 with an antimicrobial barrier formed by Prontosan Wound Gel and Prontosan Wound Gel X.18,19
The solution that helps cleanse, debride and protect against infection.
Learn more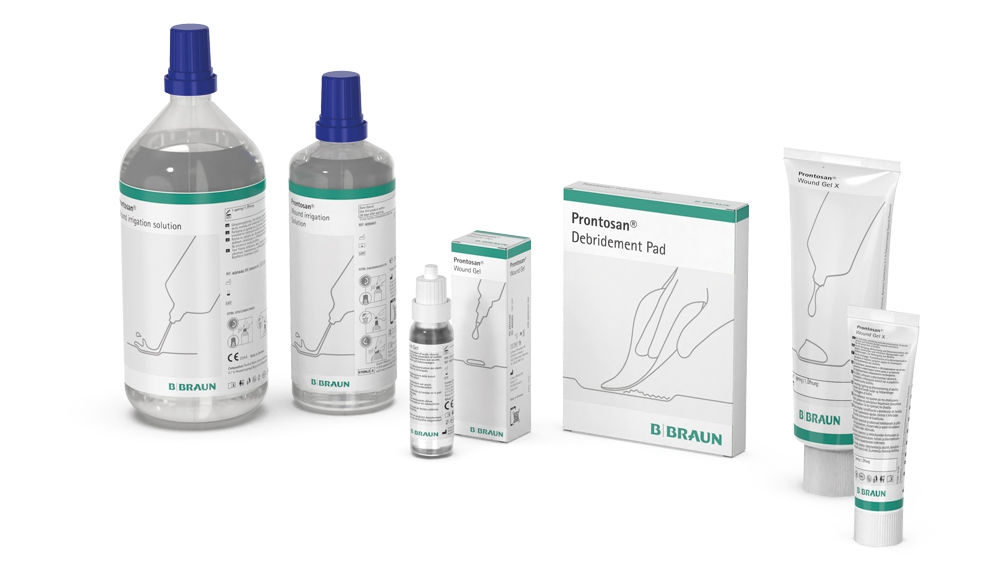
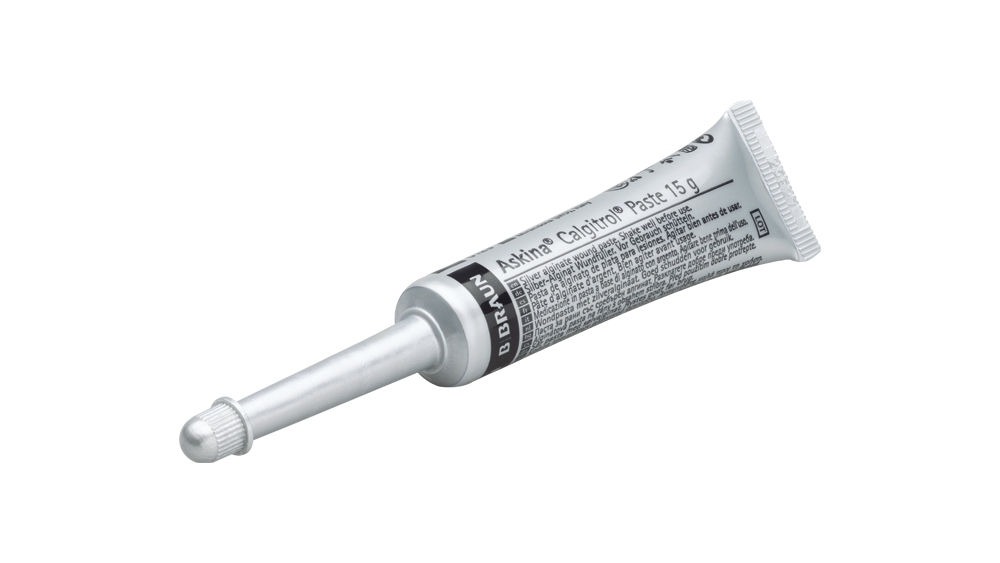
Askina® Calgitrol® Paste shows reduction of clinical signs of infection within the first week of treatment.20 while providing a broad antimicrobial effectiveness.21
Learn moreAlternative to antibiotics in infected wounds
Effective wound care begins with the right choices at the right time.
Early antibiotic use in wound management may help short-term benefits, but overuse accelerates antimicrobial resistance – a global health crisis that makes chronic wounds ever harder to manage.22 Without effective intervention, AMR could be responsible for 8.2 million deaths worldwide by 205023,24, with an economic impact up to $1 trillion25.
At B. Braun, we actively support the fight against AMR. By partnering with EWMA and sponsoring the EWMA Antimicrobial Stewardship Programme that emphasizes the prudent and appropriate use of antibiotics in wound management, we are committed to promoting best practices that preserve treatment efficacy and protect patients. Together, we can make a meaningful impact on wound care with our advanced solutions designed to promote early intervention and responsible antimicrobial practices.

All open wounds get contaminated and colonized with microorganisms; however, not all contaminated wounds become infected. The symbiotic relationship between the host and the colonizing microorganism becomes pathogenic when the host’s immune system becomes compromised by the virulence of organisms present within a wound, and wound infection occurs. Biofilms also contribute to delayed wound healing and increase the risk of wound infection.26
The risk of wound infection is influenced by characteristics of the individual (host), their wound, and the environment. Host factors that influence the development of wound infection are systemic, multifactorial and encompass many variables. The type of wound (i.e. aetiology) also contributes to the risk of infection.26
Local infection is used to refer to a stage of infection in which there is presence and proliferation of microorganisms within the wound that evoke a response from the host, often including a delay in wound healing. Local infection is contained within the wound and the immediate peri-wound region (less than 2cm). Local infection often presents as covert (subtle) signs and symptoms, that may not be immediately recognized as a sign of infection.
Covert (subtle) signs and symptoms of wound infection include: Hypergranulation, Bleeding, friable granulation, Epithelial bridging and pocketing in granulation tissue, Increasing exudate, Delayed wound healing beyond expectations. As local wound infection progresses, classic cardinal (overt) signs and symptoms that are traditionally associated with local infections generally become evident: erythema, local warmth, swelling, purulent discharge, wound breakdown and enlargement, pain and increasing malodor.26
Up to 90% of chronic wounds contain biofilm with a role in wound infection. There has been an evolving understanding and acceptance of the association between biofilms, delayed wound healing, risk of wound infection, increase antibiotic resistance.26
Prevention of wound infection is focused on implementing strategies to reduce the patient’s individual risk factors. Establishing clinical goals, working with the patient and their family, and Holistic Assessment and Management to reduce wound infection risk. In addition to an individualized approach to addressing clinical and environmental wound infection risk factors, topical antimicrobials might have a role for preventing wound infection in very high risk wounds.26
Wound cleansing is a fundamental component of wound bed preparation. Wound cleansing is defined as actively removing surface contaminants, loose debris, non-attached non-viable tissue, microorganisms and/or remnants of previous dressings from the wound surface and its surrounding skin. Therapeutic cleansing with surfactant or antimicrobial cleansers may be of added benefit in removing tenacious devitalized tissue or suspected biofilm in chronic wounds.26
Kindly check your inbox and confirm the email we've sent you.
Your feedback matters! Participate in our customer survey to help us enhance our website, products and services. Thank you for your support!